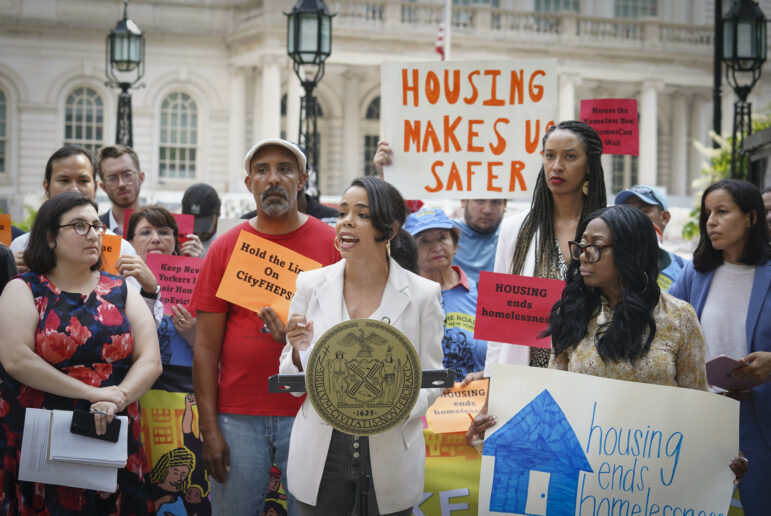Belle Lin
Montefiore Medical Center, headquartered in the Norwood section of the Bronx, is one of the busiest hospitals in the city.
Gena Bryant, a 48-year-old Bronx native, grew up without her father Gilbert Calderon in her life. So when they reconnected during her teens, she was excited that their relationship was beginning to blossom. They started talking on the phone once, sometimes twice a week. He would call just because he was thinking of her. Over the holidays, he would take the Metro-North train from the East Bronx to her Bronxville home, arms full of gifts for her two children.
In March 2017, their relationship was cut short after her father checked himself into Montefiore Medical Center’s main campus in Norwood, a neighborhood in the Bronx, just two miles from his home. They spoke on the phone while he was there. “He said he was doing well. He said he was going to be released,” she remembered.
The following day, around six in the morning, she got a call from the hospital. She found out that her father, who was 76, hanged himself in the bathroom of his hospital room.
Bryant and her husband rushed to Montefiore. They were greeted by detectives and police officers who swarmed the room, two of them talking to her at once. She was overwhelmed.
“I felt like I was on TV in one of those murder shows. It was surreal,” she said.
So Bryant was pulled aside, where a doctor told her they’d given her father “all the possible care that he needed.” But Montefiore didn’t tell her they had made mistakes.
According to a subsequent inspection conducted by the U.S. Centers for Medicare & Medicaid Services, Montefiore, the largest hospital system in the Bronx, did not conduct a follow-up psychiatric consultation after her father was found likely to be depressed after he attended a friend’s funeral. Then, nursing staff claimed they’d completed their hourly check-ups on him, but they did not — leaving him alone when the suicide occurred.
Bryant also discovered that just a week before her father’s death, another Montefiore patient had committed suicide in the exact same manner. The patient, a 77-year-old Bronx resident suffering from cancer and seeking end-of-life care, also hung himself in the bathroom of his hospital room, according to reports from CMS, as the agency is known. The reports do not name either man, but records from the city medical examiner match the dates and circumstances in the hospital inspection reports.
Over the past decade, there have been at least five suicide attempts at Montefiore, four of which succeeded, as well as other incidents where potentially suicidal patients were insufficiently supervised and had clear opportunities for self-harm. From 2016 to 2017, inspectors found that the hospital repeatedly failed to implement changes recommended by its internal committees — such as suicide training programs for nurses, environmental safety checks, and updating policy to search patients for dangerous items.
These failures, according to the report, “resulted in patient deaths.” In the 77-year-old patient’s case, Montefiore used a bed alarm system that a head nurse acknowledged had a known problem — it could be disabled by patients, thus preventing nurses from knowing when they got out of bed. In other cases, patients were placed in seclusion without a doctor’s order and remained there, unmonitored, and sharp objects were left unobserved in front of minors and patients with suicidal tendencies.
Inspectors from CMS discovered Montefiore’s recent suicide issues after the deaths, and the agency issued a warning to the hospital that included the threat of losing millions in federal funding — which could have caused it to close. In response, Montefiore filed a corrective action plan on April 2017. Since then, there have been no reports of suicides or attempts, according to federal records.
However, following its unusual number of suicides, it remains unclear whether Montefiore has fixed all the problems inspectors cited them for. The hospital refused to answer questions regarding its suicide or patient safety issues. It also declined to make a spokesperson available, and instead emailed a lengthy statement focusing on its accomplishments and regulatory compliance.
“Montefiore works closely with key oversight bodies: the Joint Commission, CMS, and the State of New York, along with the [Accreditation Council for Graduate Medical Education],” read the statement in part. “We are dedicated to cultivating physicians who are trained to promote optimal patient quality and safety.”
Some nurses at Montefiore are wary of the hospital’s promised changes. Candice Sering, a nursing union representative, said that after Calderon’s suicide, the hospital pledged to increase its level of monitoring for patients, but hasn’t committed enough staff to see it through.
A CMS spokesperson declined to comment on suicide issues at the hospital, saying that the agency does not provide comment on inspection reports.
A healthcare giant
Montefiore Medical Center was founded in 1884 by Jewish philanthropists as a facility to care for the city’s chronically ill. In 1888, it expanded to a 140-bed facility in West Harlem, and by 1912, moved from the Upper East Side to its current location in the Bronx’s Norwood neighborhood.
Since then, Montefiore has ballooned into a dominant health care player — not just the largest in the Bronx, but one of the biggest regional health care systems in the country. In 2016, its 726-bed Moses campus — where Bryant’s father was treated — was the fourth busiest in the state by total number of inpatient discharges.