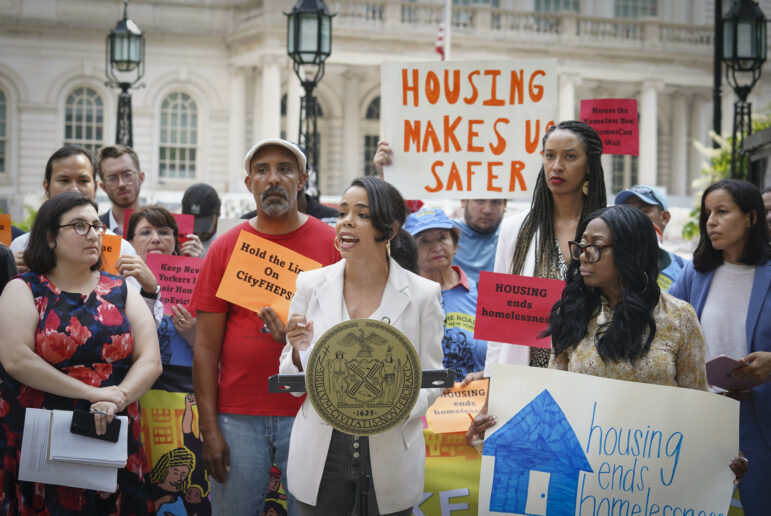Six years ago, when Empire Blue Cross and Blue Shield, New York’s largest nonprofit insurer, announced its intention to convert to a for-profit, publicly traded company, consumer and health care advocates lined up to make the best of a bad situation. Sure, the state would be losing the insurer of last resort for the poor and uninsured, but consumers and state residents would be compensated for the loss. State law required that Empire’s assets continue being applied toward its original mission–improving the availability and accessibility of health care to New Yorkers. Following the national trend in so-called “health care conversions,” Empire promised to create a foundation. With over $1 billion in assets and an independent board of directors, the foundation would put nearly $50 million each year into programs aimed at helping the poor and uninsured across the state.
“A foundation is a good mechanism for using converted nonprofit assets,” explains Phillip Gonzalez, Philanthropy Project director for Community Catalyst, a Boston-based health care advocacy group, whose report “Building Strong Foundations” is the bible of best-practices in health care conversions. “You can do a lot of specific things within a broad mandate, and it’s a good way to monetize the assets”–that is, get the proceeds from the sale circulating for the public good. The key to creating a responsive foundation, Gonzalez says, is an inclusive planning process and governance and organizational structures that are transparent and accountable to the public. “It’s got to be an open and accountable process.”
Yet the process in New York has been anything but open and transparent. After numerous public hearings, Attorney General Elliot Spitzer and Insurance Superintendent Gregory Serio had signed off on the conversion: Empire would get access to public equity markets and shed some of its regulatory burdens, and New York would get a $1 billion conversion foundation. This past January, however, Governor Pataki announced a new deal with Dennis Rivera, head of 1199/SEIU, the state’s largest union. Instead of a foundation, Empire’s assets will underwrite raises for health care workers across the state. (The union has since endorsed Pakaki’s reelection bid.) After some public wrangling, the legislature amended the plan, promising 5 percent, roughly $55 million, for a health care conversion foundation. The deal, negotiated in secret, sailed through the state legislature on a midnight vote.
“To us, this feels like a bait-and-switch transaction,” says Chuck Bell, program director of Consumers Union. “If the state brought this plan to the table in the hearings held in 1997 and 1999, it would have been a non-starter.” In August, Consumers Union and other public interest and health groups filed a lawsuit to block the conversion, challenging the legislation’s constitutionality on the grounds that it impairs an implicit contract between Empire and its subscribers vis-à-vis the organization’s charitable mission; that it takes a charitable organization’s property without a proper government purpose; and that it usurps the New York State Supreme Court’s prescribed role in reviewing and approving a conversion. “The state cannot simply take $1 billion of charitable assets that were dedicated to increasing New Yorkers’ access to health care and divert those funds to other purposes,” says Mark Scherzer, attorney for the plaintiffs.
Few observers expect Serio, a Pataki appointee, to reject the plan. But if the court overturns the legislation, Empire officials and state legislators will have to go back to the drawing board. Meanwhile, the tussle over Empire’s assets leaves important questions unanswered, ones that will become pressing as other nonprofit health care organizations, including HIP, weigh whether to follow Empire’s precedent. What is the best use of a health care nonprofit’s assets following a conversion? Is a foundation the best mechanism for dispensing those assets and securing the public’s interest? And what exactly could you do if you had a billion dollars?
_______
One thing is for sure: If the current plan is allowed to stand, New York will be an ignominious exception to a national trend. Over the past 30 years, 166 nonprofit health care organizations–hospitals, insurance plans and HMOs–have merged with or been converted to for-profit companies. According to a 2001 survey by Grantmakers in Health, health care conversions in 33 states and Washington, D.C., have created 139 new foundations with combined assets of $15.3 billion. Of these, six transactions have involved Blue Cross plans.
In the most successful cases, conversion foundations have bankrolled a broad range of activities–insurance pilot programs, community education, drug treatment, neighborhood clinics, technology, Medicaid advocacy, handgun control–aimed at creating structural reforms in health care systems, improving access, and expanding coverage. The California Healthcare Foundation provided $2.5 million to support subsidized health insurance through the state’s high risk pool, which provides health insurance to people who can’t get private coverage because of disability or chronic health conditions. Closer to home, the Healthcare Foundation of New Jersey provides almost $1 million per year to support five school-based health care centers in low-income communities. Last year, the clinics, which provide medical exams, prescriptions, immunization and oral health services, had more than 10,000 visits.
But Denise Soffel, senior policy analyst at the Community Service Society of New York, notes that even the largest foundation couldn’t begin to address New York’s health care needs. “A billion dollars doesn’t buy you universal coverage forever. So the question becomes, How can we leverage those dollars?”
California, which is home to the nation’s three largest conversion foundations, provides some ideas. Throughout the 1990s, the California Endowment and the California Wellness Foundation emerged as statewide leaders for improved public health programs and expanded access–and as national models for conversion foundations.
In 1992, the California Wellness Foundation launched the Violence Prevention Initiative, a major initiative aimed at reducing youth access to firearms, increasing public support for youth violence prevention programs, and reducing youth access to alcohol and other drugs. The foundation invested $14 million in a public education campaign and in its first decade helped boost state funding for violence prevention from $8 million to $390 million. Wellness grantees formed the backbone of coalitions that led at least 60 cities to enact firearms regulations.
“There are two things that we can do that government can’t do,” explains Dr. Robert Ross, president and CEO of the California Endowment. “First, we can focus our advocacy on the truly marginalized and voiceless populations. Second, we can take the long view: It’s not in the physiology of elected officials to look past the next election. These are not two- to three-year projects. We are in this for the long haul.”
Since its inception in 1996, the $3.4 billion California Endowment has focused on prevention and access for California’s increasingly diverse population. This past April, the foundation announced a five-year, $20 million program to increase health coverage among the 1.7 million residents of Los Angeles County who are eligible for public insurance but not enrolled. The grant included $9 million for community-based organizations to improve outreach and enrollment; $3 million for local policy and advocacy work; and $1.5 million for a public awareness campaign. Over the next five years the California Endowment, in coalition with other nonprofits and foundations, hopes to achieve 100 percent coverage for children and their families throughout the state.
_______
An Empire conversion would give New York the second-largest health care conversion foundation in the country, slightly larger than the California Wellness Foundation. Still, it’s not the size of a foundation’s assets that matters, but what it does with them.
By and large, health care advocates would like to see those funds channeled into two issue areas: insurance and access. According to a 2001 study by the United Hospital Fund, 19 percent of all New Yorkers, and one in four New York City residents, lack health insurance. Of the three million statewide without health insurance, the report estimates, fully half are eligible for Medicaid, Family Health Plus or Child Health Plus.
State officials say they are doing enough to meet insurance needs. “New York has, more than any other state, I believe, already created programs to address the problems of the uninsured,” Robert Hinckley, the state health department’s director of operations, told the New York Times. “Funding for these programs is sufficient and solid.”
Health care advocates, on the other hand, argue that the gap is a sign that the state could be doing more to ensure low-income residents take advantage of public insurance programs. In the four months following the World Trade Center attacks, 350,000 uninsured New Yorkers signed up for Disaster Relief Medicaid–10 times the usual enrollment rate. The jump was largely due to simplicity: the application was one page, and the only documentation required was proof of identity. As those benefits run out, however, 30 to 50 percent of the new beneficiaries may be kicked off because even though they are eligible, they can’t navigate the Byzantine regular enrollment process.
A conversion foundation, advocates argue, would be perfectly suited to funding the outreach and advocacy necessary to bridge these gaps. For example, if more than 1 percent of residents in a hospital’s community speak a language other than English, the state hospital code and federal law require the hospital to provide interpreters and translated documents in the language. The last time the state health department publicized that requirement–much less enforced it–was 1988. “This money could go towards improving health care or expanding insurance coverage,” says Judy Wessler, executive director of the Commission on the Public’s Health System. “But instead the money is going to be pissed away.”
_______
On the other hand, some critics contend, conversion foundations are equally capable of pissing money away. “Conversion foundations are a mixed bag,” says Lance Lindblom, president of the Nathan Cummings Foundation. The same independence that gives foundations the ability to fund advocacy and public health activities that might not receive public dollars can also lead to a lack of public oversight and accountability. A billion-dollar foundation will tie up 95 percent of its assets in an endowment, and while it will pay out $50 million per year, a significant portion of that goes toward expensive staff and asset managers. And while some foundations have funded aggressive advocacy and efforts to expand access, many others have been content to fund medical research and academic papers. “Ultimately, a foundation’s effectiveness depends on where the money will go and who controls it,” says Lindblom–making community oversight and board governance paramount issues.
On that front, New York’s plans portend badly. Under the current plan, the new mini-foundation would be governed by a nine-member board of directors–three voting members and six nonvoting members. The governor, the president of the State Senate, and the speaker of the Assembly each get to appoint a voting member and two nonvoting members. Consumer activists managed to squeeze in some feel-good language about the board including representatives from consumer groups, patients, and public health experts, but the governance structure virtually guarantees at best a bland mission, and, at worst, a grist mill for political patronage. Although the foundation’s mission will include expansion of access to care, better delivery of care and health education, the three voting members must agree unanimously to every grant, rendering the foundation as decisive and audacious as the U.N. Security Council.
What’s more, Empire’s conversion will set a precedent for future conversions. If the state is allowed to expropriate charitable assets to plug its budget gaps, what’s to stop state officials from siphoning off nonprofit assets from elsewhere–hospitals, museums, public parks? “The whole idea of [the Pataki deal] was that the government could accomplish many of its budgetary priorities with very little concessions in the way of taxes or spending cuts,” suggests plaintiffs’ attorney Mark Scherzer. “That’s what made it such an attractive plum to pick off the tree. But unfortunately, you can’t go around picking other people’s plums.” And once the low-hanging fruit is gone, what will be left of the public’s assets?